Introduction
Muscle strain is one of the most common injuries in sports. As a physical therapist, I have seen many athletes who returned to sports with no or minimal rehabilitation. Once the pain goes away, can we just return back to sports? ABSOLUTELY NO. After muscle injury, the muscle is much weaker and stiffer than before the injury. Even if you feel okay, your muscle is still damaged. You must complete muscle strain rehabilitation program before going back to sports. Even after strength comes back, you have to assess whole body movement with a physical therapist or athletic trainer to find a cause of the injury. Otherwise, you will highly likely have another injury in the future. In this blog, I introduce general information about hamstrings injury and its rehabilitation program by using hamstrings injury guideline and other research articles as reference.
How do we get muscle injury?
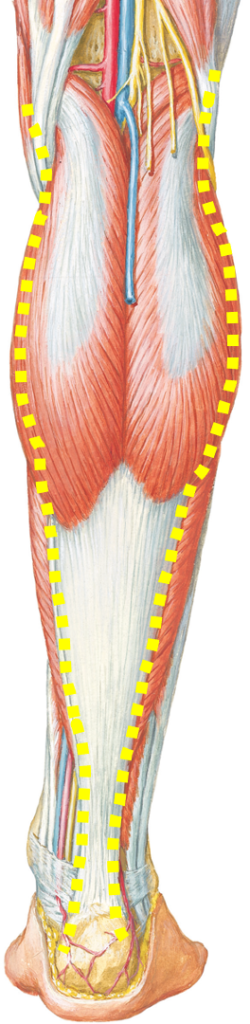
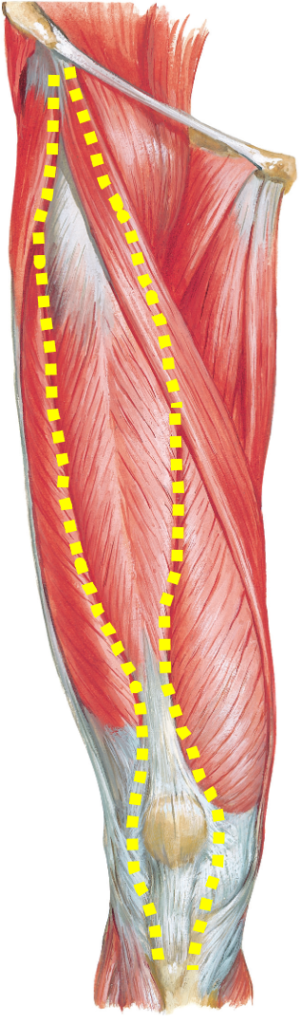
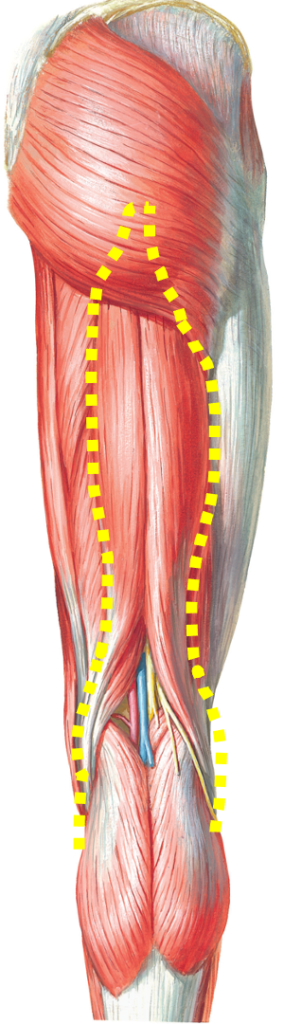
Gastrocnemius
Rectus Femoris
Hamstrings
(usually biceps femoris)
The muscles shown above are the three main muscles to get strain. Due to the anatomical feature, muscles crossing two joints are susceptible to muscle strain. Gastrocnemius crosses ankle and knee joints. Hamstrings cross knee and hip joints. Rectus femoris also crosses knee and hip joints. When you put too much stress on those muscles while movement due to poor body control, the muscles would get injured. Especially, hamstrings are the most common muscle injury site because hamstrings work a lot and also easily get stretched during sports activities.
Muscles injury usually happens in the muscle-stretched position during high-velocity movement. For example, when we sprint, we bend our hip and straighten knee which stretches hamstrings in the air before landing. Gastrocnemius gets damaged when you push off the ground knee straightened (muscle stretched). If you do not have a good muscle control during high-velocity movement, those muscle fibers get damaged.
Who has high risk of muscle injury?
- History of muscle injury
- Older than 23 years old
- Playing sports demanding high speed running (soccer, football, rugby, track&field)
These are the risk factors noted in the guideline. If you have had muscle injury in the past, you have higher risk to have another one compared to the people who have not. In addition, as you get older, your strengths, flexibility, and athletic skills start to decline. You should be careful if you are an adult. Finally, in many cases, muscle injuries happen during high speed movement. Playing sports which demands sprint would increase risk of muscle injury.
Surprisingly, poor hamstrings flexibility and strength are NOT risk factors based on the research. Instead, several articles showed that poor body control such as abnormal pelvic position and lack of abdominal activity during sports would be potential risk factors for hamstrings injury. Therefore, whole body assessment and training are required to prevent from the future muscle strain. However, after the injury, the injured muscles get weak. In that case, you must do hamstrings strengthening and stretching exercises before return to sports.
Whole body assessment
Pelvic position
Pelvic position strongly influences on tension in the hamstrings because pelvic position directly changes hip position (Hamstrings cross hip joint). Pelvic position changes depending on the muscle activity and tightness. Once your pelvis tilts too anteriorly (forward) or posteriorly (backward) during movement, hip position would be also changed, which leads the muscles to produce less force since muscle fibers are too shortened or stretched. This is explained below with length-tension curve. Thus, even if you have strong hamstrings, inappropriate pelvic position during sports activity would limit your hamstrings performance, which causes muscle injury. How hamstrings are stretched with anterior pelvic tilt is explained in the video on the top of the page.
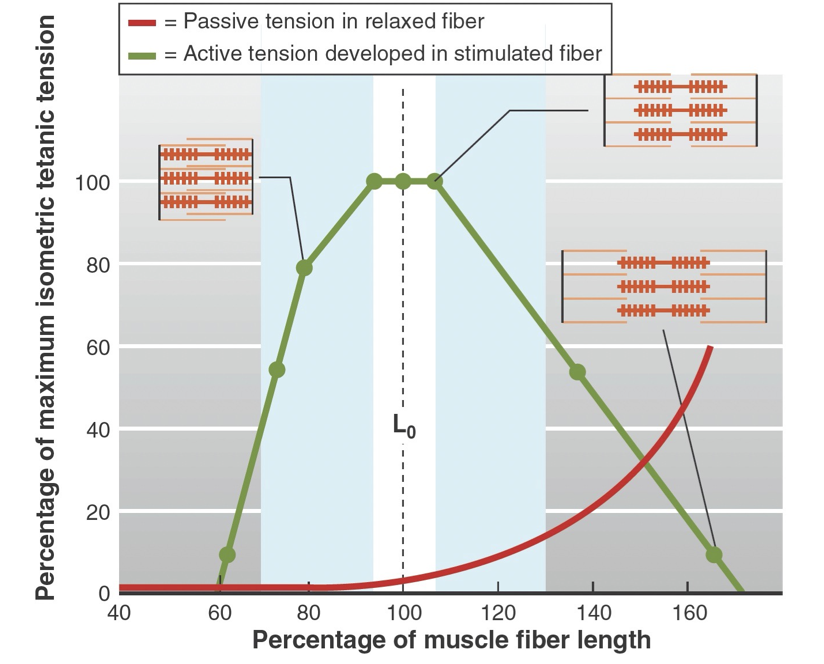
Length-tension curve
Please look at the green line.
- Once the muscle gets stretched (on the right side), force production from muscle decreases because muscle fibers are not able to pull together.
- Once muscle gets shortened (on the left side), force production also decreases because there is no potential space to shorten the muscle fibers anymore.
- Thus, middle range would be the best position for the muscle to produce force from muscle contraction.
Where is the appropriate pelvic position?
We need to set up appropriate pelvic position for good leg (hip) control. Proper angle of the pelvic tilt in standing is 30 degrees tilted anteriorly. To test your angle of pelvic tilt, you may place your fingers on your pelvis. Usually the height difference between posterior part of the pelvis (PSIS) and the anterior part of the pelvis (ASIS) is around 2 fingers width. If you have a good pelvic control during sports activity, your muscles work properly, which leads you to do better performance. The instruction is described below.
ASIS
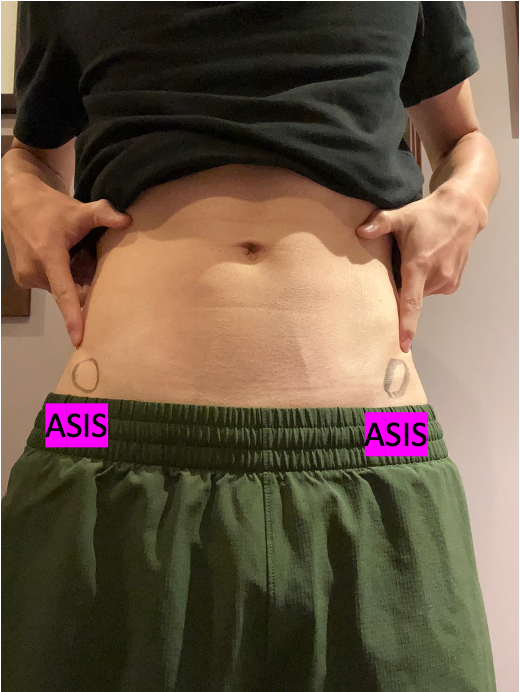
PSIS
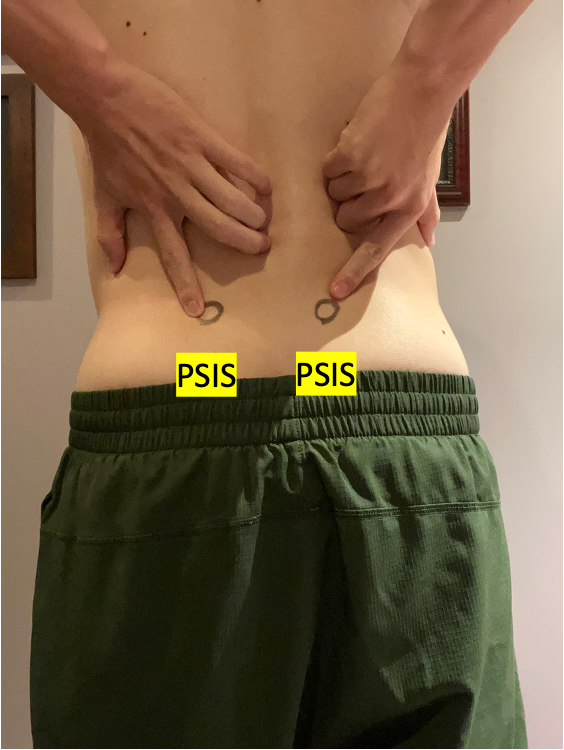
2 finger width
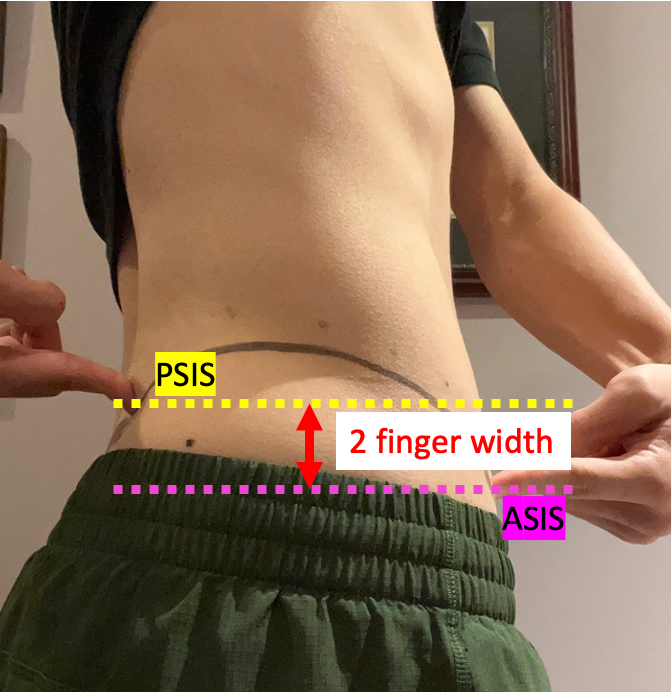
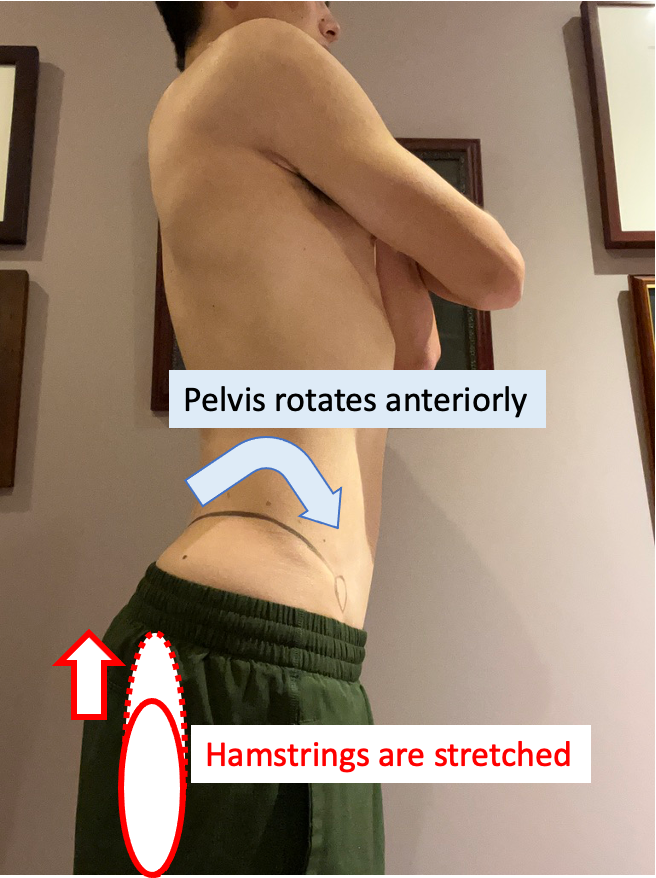
Anterior Pelvic tilt
If the pelvis is anteriorly tilted in standing position, the hamstrings are stretched and usually weak due to lengthened muscle fibers. During sports activity, the further stretching is applied to the already stretched hamstrings, and muscle fibers get damaged.
Posterior pelvic tilt
If the pelvis is posteriorly tilted in standing, your hamstrings may be tight, or you may not use muscles properly. Once tight muscle gets stretched during sprint (anterior pelvic tilt), the quick stretch would cause muscle damage.
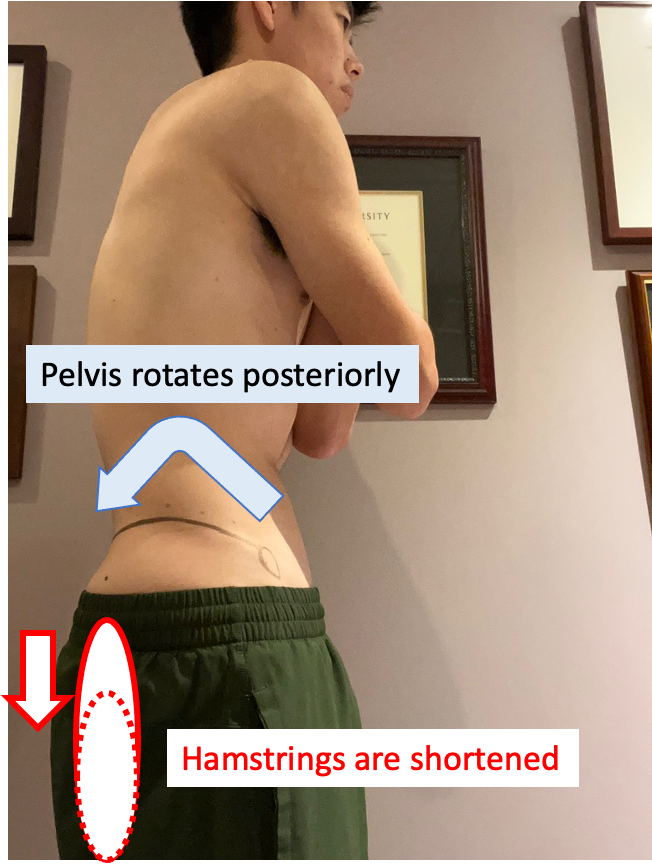
There are so many causes of having abnormal pelvic tilt. In general, quadriceps and iliopsoas tightness, back muscle tightness, weak abdominal muscles, and weak hamstrings are the contributors of the anterior pelvic tilt. Tight hamstrings, tight abdominal muscles, sway back posture (rounded back), weak back muscles may cause posterior pelvic tilt. Usually, multiple factors influence on the pelvic position. Therefore, it is difficult to figure out what is causing your abnormal pelvic position by yourself. You should visit and ask a physical therapist how your pelvic position looks.
Asymmetry
Abnormal pelvic tilt may be seen only on one side. Based on the PRI concept (Postural Restoration Institute), because of larger diaphragm on the right side and liver is placed on the right side, right side of the body is heavier than the left. As a result, people tend to put their weight on their right leg more than the left leg. Even if you think you stand on the left leg more than right, you unlikely use your muscles on the left properly in standing. In theory, if you are in that pattern, left side of the pelvis would be anteriorly tilted while right side of the pelvis is posteriorly tilted. As a result, left side of the hamstrings likely get injury due to their stretched position in standing. If you have recurrent hamstrings injury, there is something that contributes to your asymmetry or abnormality that you have not worked on yet. Please do not hesitate to reach out to a physical therapist and find what caused your recurrent muscle injury.
Pelvic asymmetry
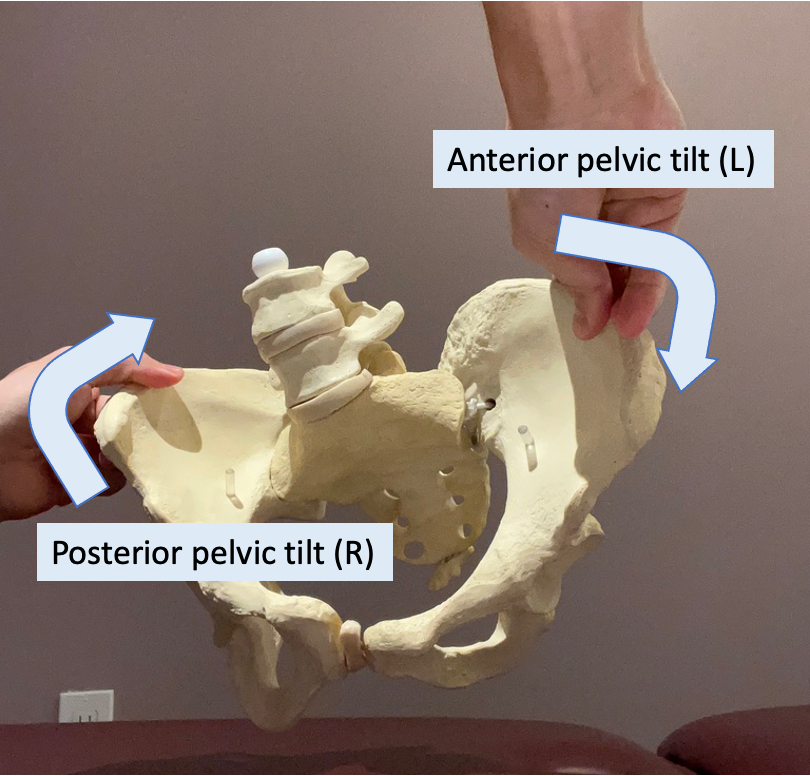
Prevention program
The guideline suggests that athletes should complete proper warm-up, stretching, core stability exercises, and balance exercises before sports activity to prevent from hamstrings injury. You should take enough time to get ready for a competition.
Another evidence-based prevention program is the Nordic Hamstrings Exercise (NHE). NHE is well-researched exercise and evidence supports its effectiveness to prevent from hamstrings injury. An example of NHE program is shown on the right. This exercise has high intensity for hamstrings. Thus, you may start with 5 sets of 2 reps (total 10 reps), then progress weekly to 10 sets of 3 reps (total 30 reps).

Rehabilitation program
There are three different level of the injury: mild (grade 1), moderate (grade 2), and severe (grade 3). This time, I focus on moderate (grade 2) level of injury in the muscle-tendon junction which is common site of the strain injury. Duration of each phase depends on the individual, so you may not completely follow these durations.
Acute phase (0-5 days)
The goal of the rehabilitation program in the first week is to walk without pain. If you still feel pain with walking after 1 week, you should not progress to the next phase of the program. In acute phase, you should avoid stretching muscles because the injured muscle fibers are vulnerable to mechanical stress at that point, so that may aggravate pain. As a rehabilitation program, icing, isometric training, range of motion exercise, and gait training are self-care exercise that physical therapists would recommend. All of these exercises have effect of pain relief. You should also keep strengths in other parts of the body, such as the opposite side of the leg, trunk, and ankle. Physical therapists also apply manual therapy to decrease stiffness caused by internal scar tissue in the muscle fibers. You should never wait for pain relief with rest and just return to sports, which many athletes do. Exercise details are explained in the video.
Icing
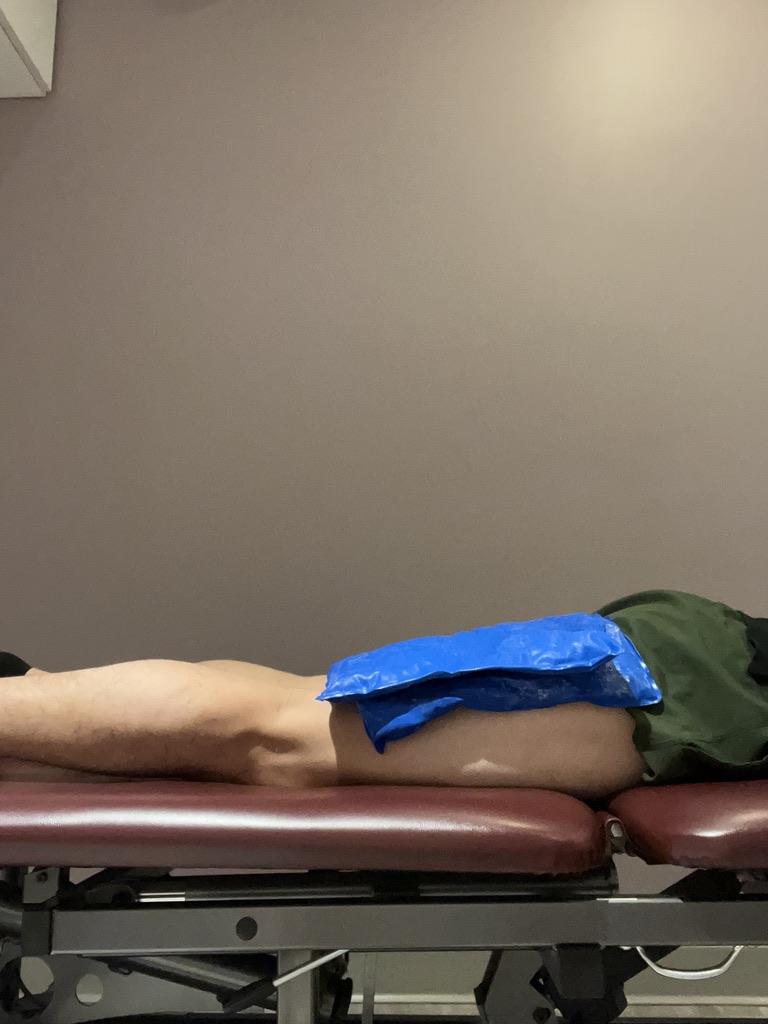
Isometric training

Range of motion
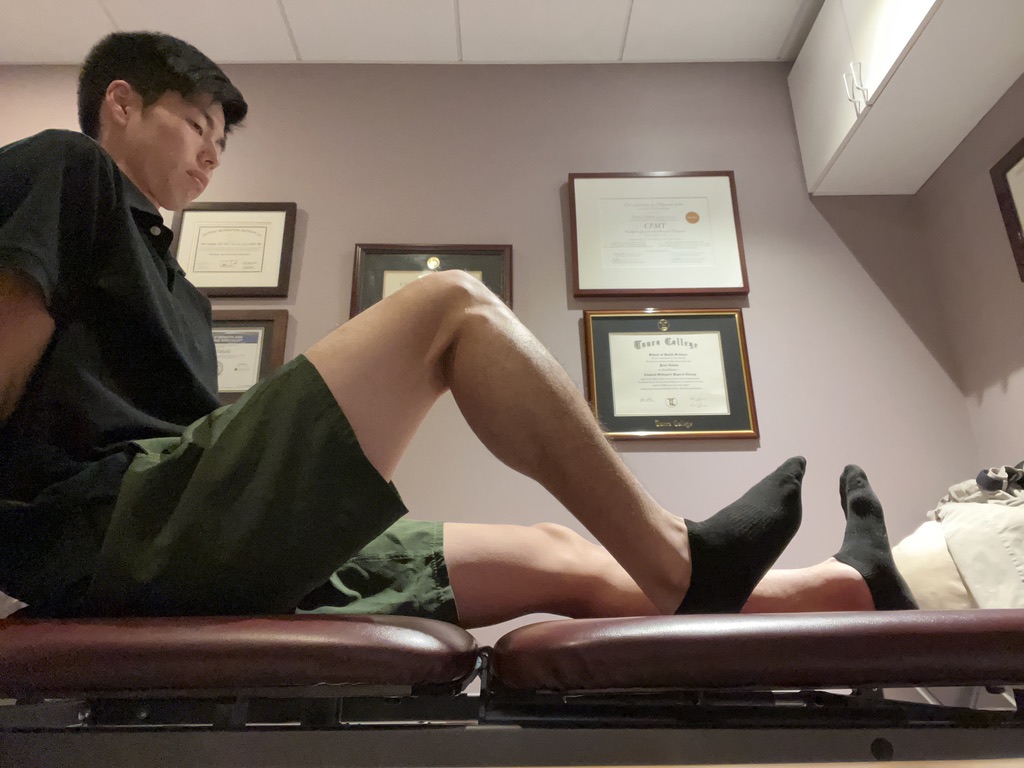
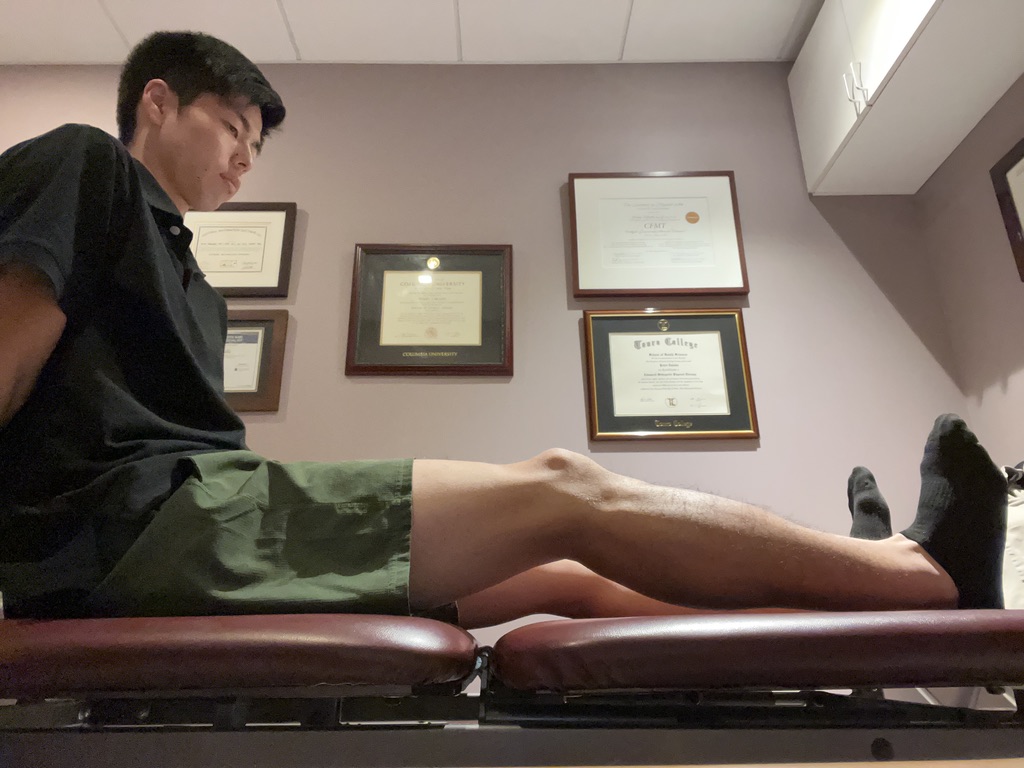
Remodeling phase/subacute phase (5-14 days)
By the end of the remodeling phase, you should be able to have full range of hamstrings motion, pain-free hamstrings contraction, and pain-free 75% of sprint. In this phase, you may do hamstrings stretching, hamstrings strengthening with weight, and start jogging and running. Please make sure you progress exercise intensity gradually. If you progress exercise too quickly, you may have more pain with damaging muscle fibers, which delays rehabilitation program. Having pain during or after exercise means that the muscle is not ready for the exercise intensity. Be aware that there is no fast-returning program. Even if you feel fine, the muscle fibers are still recovering, so you need to complete proper rehabilitation program before return to sports.
Hamstrings stretching
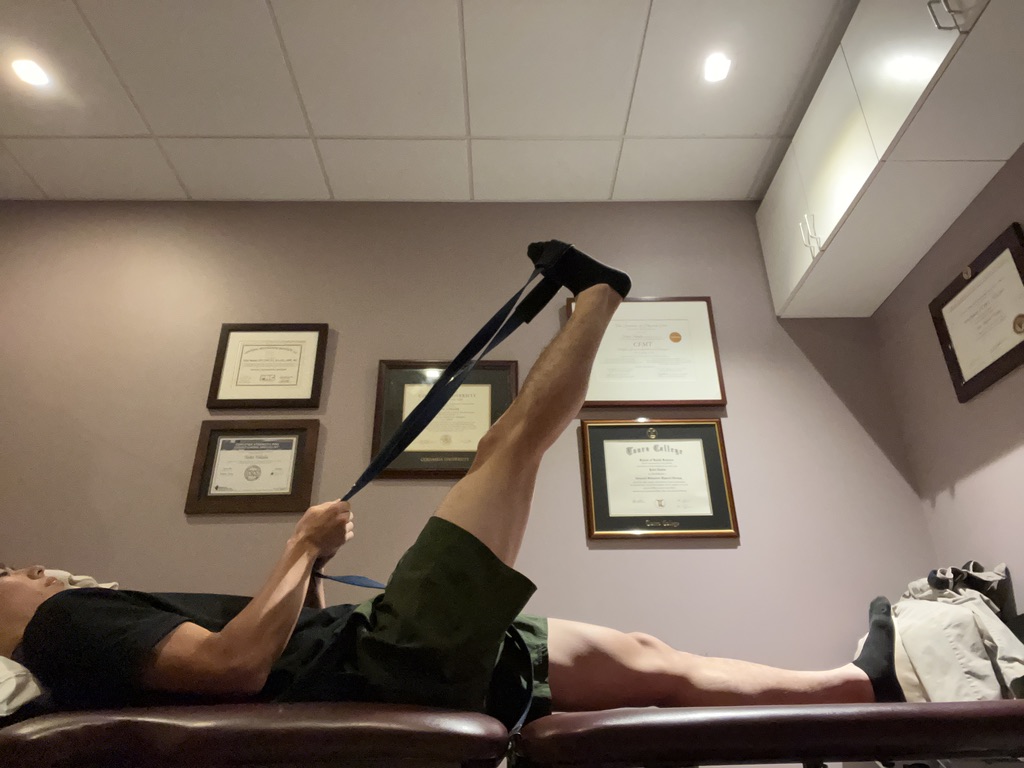


Hamstrings strengthening
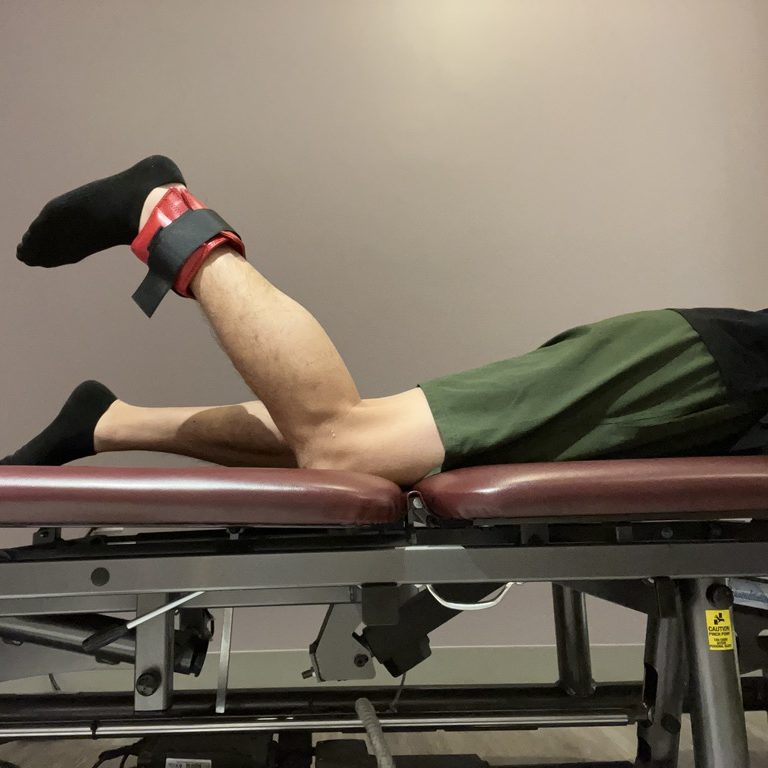



Jump exercises


Functioning phase (14-28 days)
Finally, muscles are ready to do some sports activities. Strong collagen fibers (type I) around the muscle are made by early in the third week, and muscle regeneration is completed by the end of the third week. Thus, at the end of this phase, muscle fibers should be recovered. At this point, you should not feel pain nor weakness in any movement. The goal of this phase is to return to sports with minimal risk of re-injury. You may keep doing hamstrings strengthening and stretching as prevention program. Physical therapists focus on sports-related field movements such as agility, cutting, sprint, and jump. Again, you should progress exercise intensity very carefully. Once you get full strength, balance, flexibility, and good body control, then you are all set!!
Conclusion
What I explained above is general muscle strain rehabilitation program. Each person has different issues in the body. Throughout the rehabilitation process, your whole-body control should be checked before return to sports because any small imbalance may cause another muscle strain. Hamstrings programs may not be enough to prevent from muscle strain. Again, a whole-body assessment and conditioning are required to prevent from hamstrings injury. Even if you think you have good physical performance, you may not realize your asymmetry or weaknesses. Please do not hesitate to ask your trainer or visit physical therapy clinic (my recommendation is FuncPhysio 😀).
Reference
- Hamstring strain injury in athletes. J Orthop Sports Phys Ther 2022;52(3):CPG1–CPG44. doi:10.2519/jospt.2022.0301
- Vander’s Human Physiology The mechanism of body function. Widmaier,EP., Raff,H., Strang,KT. forteenth edition. 2016
- Netter, FH. Atlas of Human Anatomy. 6th edition. 2014
- Hamstrings rehabilitation in elite track and field athletes: applying the British Athletics Muscle Injury Classification in clinical practice. Macdonald, B., McAleer, S., Kelly, S., et al. Br J Sports Med. 2019 Dec;53(23):1464-1473.
- Hamstring Strain Injury Rehabilitation. Hickey, JT., Opar, DA., Weiss, LJ., et al. J Athl Train. 2022 Feb 1;57(2):125-135.
- Effects of Nordic Hamstring Exercise on Hamstring Injuries in High School Soccer Players: A Randomized Controlled Trial. Hasebe, Y., Akasaka, K., Otsudo, T., et al. Int J Sports Med. 2020 Mar;41(3):154-160.


