Tempromandibular dysfunction, TMD
Temporomandibular dysfunction (TMD) is a disorder that involves the jaw muscles, the temporomandibular joint, and nerves causing facial pain. TMD is caused by a complex system of muscles, bones, joints, and other structures that do not work together harmoniously.
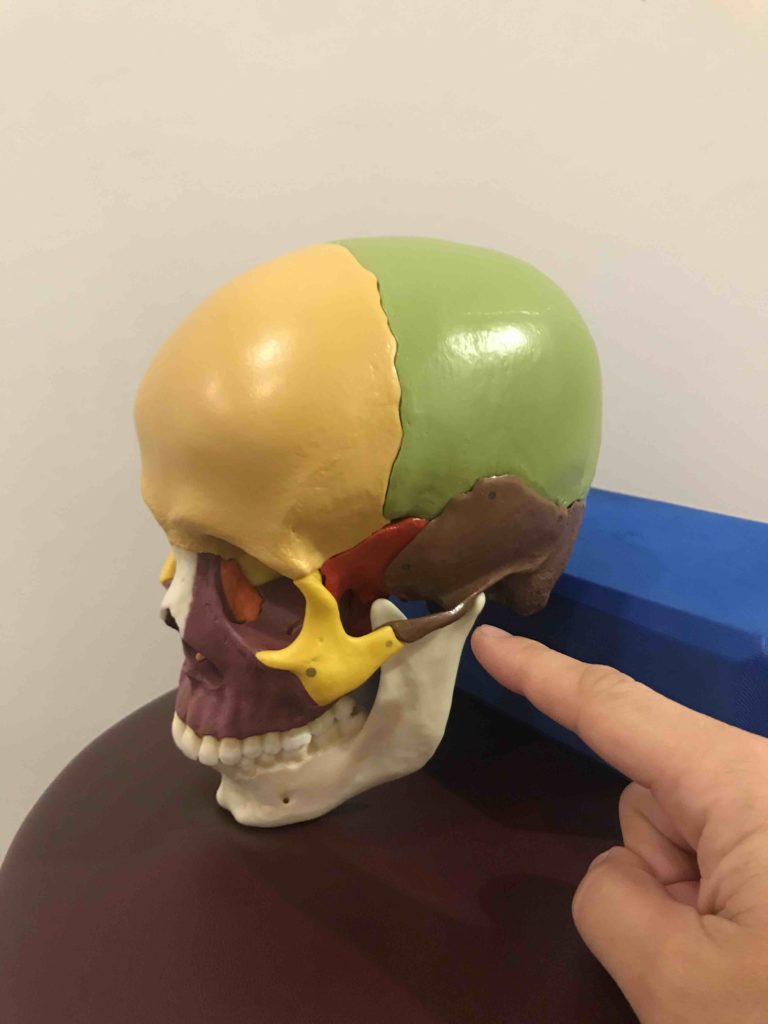
Tempromandibular dysfunction or disorder (TMD) is a condition that affects the muscles of the jaw, the temporomandibular joint (TMJ), and facial pain. TMD is caused by the failure of the complex system of muscles, bones, and joints to work together properly. When the jaw and the joint are properly aligned, smooth muscle activities such as chewing, talking, yawning, and swallowing are carried out. However, when these structures (muscles, ligaments, discs, jawbone, and temporal bone) are misaligned, and the movements are not synchronized, several problems may arise. There are several classifications of TMD, but I believe they can be mainly divided into the following three patterns:
- Myofascial pain: This is the most common form of TMD and causes discomfort or pain in the muscles or fascia that control chewing, neck, and shoulder function. It can manifest symptoms similar to those of neck and shoulder stiffness.
- Joint derangement: This includes disorders of the disc (a cushion of cartilage between the jawbone and the skull) between the joints or bone problems of the jawbone that cause jaw dislocation.
- Degenerative joint disease: This includes conditions such as arthritis and rheumatoid arthritis of the temporomandibular joint.
Of course, many people may suffer from one or more of these conditions simultaneously.
The cause of TMD cannot be pinpointed to one specific factor, but excessive stress on the temporomandibular joint is undoubtedly a significant contributor. For example, teeth grinding or clenching is a common cause. This strain may be a result of bruxism. Stress is also a common factor in causing teeth clenching and grinding, leading to TMD. However, trauma to the jaw, head, or neck can also cause TMD. In addition, painful conditions such as fibromyalgia and irritable bowel syndrome may exacerbate TMD pain. Therefore, TMD is believed to be caused by orthopedic, psychological, sensory, genetic, and neurological factors.
The signs and symptoms of TMD are as follows. If you have any of these symptoms, please consult with FuncPhysio:
- Jaw discomfort or soreness (often most prevalent in the morning or late afternoon)
- Headaches
- Pain spreading behind the eyes, in the face, shoulder, neck, and/or back
- Earaches or ringing in the ears (not caused by an infection of the inner ear canal)
- Clicking or popping of the jaw
- Locking of the jaw
- Limited mouth motions
- Clenching or grinding of the teeth
- Dizziness
- Sensitivity of the teeth without the presence of an oral health disease
- A change in the way the upper and lower teeth fit together
The symptoms of TMD may look like other conditions or medical problems. FuncPhysio works in conjunction with dentists and physicians to provide appropriate treatment for TMD.

Many cases of TMJ disorders are caused not by problems with the joint itself but by stress from imbalances in other parts of the body. These imbalances can be due to posture, balance issues in the body, problems with the cervical spine (such as a straight neck), stiffness in the chewing muscles (imbalance), breathing problems, autonomic nervous system problems, and more. At FuncPhysio, we have achieved fundamental improvements in many TMJ disorder patients by improving these conditions through manual and movement-based therapy.
Headache
Headaches are a very common complaint. The estimated global prevalence of active headache disorder was 52.0%. More than half of the population suffers from some sort of headache.
The International Classification of Headache Disorders defines more than 150 different types of headaches, which it divides into two main categories: primary and secondary.
Of course, certain headaches are life-threatening, and you need immediate medical attention. However, many types of headaches are triggered by underlying physical conditions that could be managed by physical therapy. For example, migraines are triggered by stress and anxiety, bright lights and loud noise etc. And it is true that once migraine headaches get triggered, there might not have the way of treatments.
But migraine triggers are often associated with the cranial pattern (torsion), imbalance in the sympathetic and parasympathetic system, tension in the cervical and thoracic region, disturbance in the craniosacral system, and so on. These factors can manage by physical therapy.
1, Stovner LJ, Hagen k, Steiner TJ. The global prevalence of headache: an update, with analysis of the influences of methodological factors on prevalence estimates: J of headache and pain;23:34(2022)
Tinnitus(Ear Ringing)
Tinnitus, or ringing in the ears, is a symptom that has many causes and is difficult to pinpoint. In fact, tinnitus and dizziness are probably the most searched for symptoms on the Internet. The search suggests that it occurs when the areas of the brain involved in hearing spontaneously increase their activity. Therefore, it is not an exaggeration to say that it is associated with almost all disorders of the auditory system. It is not limited to ringing in the ears, but may be perceived as whistling, buzzing, humming, hissing, roaring, chirping, and many other sounds.
There are three forms of tinnitus, which are briefly described here. The first and most common form occurs from damage to the inner ear or cochlea (Cochlea) due to exposure to high volume sound.
The second common form of tinnitus is stimulation of the autonomic nervous system from increased neuromuscular tension. Retraining therapy helps reduce this tension from the autonomic nervous system, a process that usually takes two or more years. This process is referred to as habituation of the response. Such retraining, however, becomes impossible when the symptoms are threatening, negative experiences, undiagnosed, or in situations where the individual is under a lot of emotional stress. Many tinnitus sufferers have a high degree of sensitivity to external sounds and often seek out and seek out quiet environments to work in. However, this too can have a negative effect. This is because the subconscious survival style or state response mechanism will always be concerned about tinnitus because of the situation of tinnitus or being concerned about it. This often prevents the condition itself from improving.
Other symptoms that sometimes appear with tinnitus, such as emotional distress, depression, dizziness, and insomnia, are thought to be possible problems with limbic structures.
Third, there is a known relationship between tinnitus and people who suffer from TMJ disorder, teeth grinding, and limited jaw movement. These individuals may have tinnitus due to overactivity of the muscles that attach directly to the temple bone that surrounds the inner ear. At this time, the relationship between tinnitus and lateral or medial rotation of the temple bone is not clear in the literature, but a third cause directly associated with tinnitus is known to include auricular heterotopia, temporomandibular joint disorder, chewing disorder, and mouth opening restriction. This reason is said to be related to the tensor tympani muscle, which attaches to the sphenoid and temple bones. This muscle tenses the tympanic membrane and, when placed in a stretched position, can affect innervation by the mandibular branch of the trigeminal nerve. This can have a direct effect on the outer surface of the eardrum and cause tinnitus.
The causes of tinnitus are many and varied, but recovery is expected as long as there is no tissue damage. As mentioned above, the majority of tinnitus is often derived from TMJ disorder, sphenoid bone distortion, muscle tension from autonomic problems, and skull distortion from postural distortion. At FuncPhysio, we often treat patients who have suffered from tinnitus for many years, and in a great many cases, the longstanding tinnitus has disappeared as a result of treatment.
A research Paper supports an Interdisciplinary (Dentist&Physical Therapist) approach to improve TMD.
“Craniovertebral and Craniomandibular Changes in Patients with Temporomandibular Joint Disorders after Physiotherapy Combined with Occlusal Splint Therapy: A Prospective Case Control Study” is a comprehensive research paper that investigates the effects of a combined treatment of physical therapy (physiotherapy) and occlusal splint therapy on patients diagnosed with temporomandibular joint disorders (TMD).
Key aspects of the study include:
Background and Objectives: The aim was to assess craniovertebral and craniomandibular changes in patients with TMD after undergoing combined physiotherapy and occlusal splint therapy.
- Combined therapy significantly affected the vertical and sagittal position of the mandible and the width of the functional space between the first and second cervical vertebrae (C1 and C2).
- Additionally, cervical lordosis was restored after treatment.
- These changes were not observed in the control group, indicating the effectiveness of the combined therapy in treating TMD.
Conclusions: The study concludes that collaboration between physiotherapists and dental practitioners is crucial in treating patients with TMD, including those with temporomandibular joint osteoarthritis. The combined treatment approach led to significant changes in the craniovertebral and craniomandibular regions, highlighting the importance of a multidisciplinary approach in managing TMD. The paper provides detailed insights into the methodology, analysis, and implications of this treatment approach, offering valuable information for medical professionals dealing with TMD.